table of contents
IPD (Inpatient Department) claims cover hospitalizations where a patient is formally admitted for 24 hours or more, requiring a full set of clinical and administrative documents, including discharge summaries, operation notes, and hospital bills. OPD (Outpatient Department) claims cover consultations, diagnostics, and pharmacy visits without overnight admission, requiring a shorter but equally precise document set including prescriptions, clinic receipts, and lab reports.
Why One Missing Document Costs Your Team the Entire Claim
According to the IRDAI Annual Report 2023-24, 11% of all health insurance claims were rejected in FY2023-24, amounting to Rs 15,100 crore in disallowed payouts. TPAs handled 72% of those 2.69 crore total claims processed that year. By FY2024-25, rejected claims had grown to Rs 30,000 crore, a 15% jump that IRDAI is now addressing through a strict new code of conduct. The primary keyword in every rejection report is the same: documentation.
For IPD vs OPD claims, the document checklist is not a formality. It is the mechanism by which TPAs adjudicate, approve, and pay. A missing discharge summary or an unsigned claim form puts the entire file into a query loop, adding 15 to 30 days to settlement time and burning adjuster hours that could be spent on complex cases.
This guide gives your team the complete reference: 25 document classes for IPD claims, 15 for OPD, a side-by-side comparison, the top rejection reasons, and how AI-powered platforms like InterPixels eliminate manual triage entirely.
“When documentation aligns, TPAs process 98% of clean claims within 30 days. When it does not, every stakeholder pays the price.”
What Is the Difference Between IPD and OPD Claims?
An IPD claim is triggered when a patient is formally admitted to a hospital for at least 24 hours. An OPD claim covers any medical interaction consultation, diagnostic test, or pharmacy purchase that does not require overnight admission. This threshold distinction drives every document requirement downstream.
In practice, teams find that the hardest misclassifications occur in day-care procedures (less than 24-hour surgeries), domiciliary treatment (home care), and teleconsultation claims. Each of these sits at the boundary between IPD and OPD rules, and each requires a specific subset of the checklists below.
The clinical pathway for IPD runs from admission through discharge, generating a trail of documents at each stage: pre-authorisation, treatment records, operating notes, pharmacy logs, and final billing. OPD is a single-visit event, but the document requirements are more precise because there is no discharge summary to anchor the claim.
The Complete IPD Claims Document Checklist (25 Document Classes)
IPD claims require up to 25 document classes covering the full hospital stay, from admission to post-discharge settlement. Every class below must be present in a complete file before adjudication can begin.
Core Clinical Documents (IPD)
- Hospital Bill (itemised, stamped, signed by billing department)
- Discharge Summary (signed by treating physician, includes diagnosis, treatment, and follow-up instructions)
- Operation / Procedure Notes (mandatory for all surgical claims; must include surgeon name, procedure date, and anaesthesia type)
- Indoor Case Papers / Patient Case File (complete inpatient record from admission to discharge)
- Investigation Reports (lab results, imaging reports, pathology reports ordered during admission)
- Pharmacy Bills (all medications dispensed during the IPD stay, itemised with batch numbers)
- Doctor Consultation Notes (each treating specialist’s progress notes)
- Anaesthesia Record (for all surgical and procedure claims)
- ICU / HDU Charts (if intensive care was provided, including vitals log and nursing notes)
- Vaccination Certificate (mandatory for post-exposure prophylaxis claims, e.g., anti-rabies)
Administrative and Identity Documents (IPD)
- Duly Completed Claim Form (insurer- or TPA-specific form, all fields filled, dated, and signed)
- Pre-Authorisation Letter (cashless claims: the TPA-issued approval must accompany the final bill)
- Room Receipt / Room Rent Evidence (daily room charges, room category, occupancy dates)
- Ambulance Receipt (if emergency transport was used; must show origin, destination, and amount)
- KYC Documents of Insured (government-issued photo ID: Aadhaar, Passport, or PAN card)
- Policy / Member ID Card Copy (confirms active coverage at date of admission)
- Insured’s Bank Account Details (for reimbursement claims; cancelled cheque or passbook copy)
- GISPA Declaration (Group Insurance Scheme Personal Accident declaration, required by specific group policy types)
- Settlement Letter (for claims involving third-party liability, accident, or workplace injury)
Special Scenario Documents (IPD)
- Death Summary (mandatory for mortality claims; includes cause of death, attending physician signature)
- Post-Mortem Report (required when the cause of death is unnatural or disputed)
- FIR / MLC Certificate (First Information Report or Medico-Legal Certificate for accident, assault, or poisoning claims)
- Newborn Birth Certificate (for maternity claims covering the neonate)
- Implant Sticker / Device Invoice (for orthopaedic, cardiac, or ophthalmic device claims; must include serial number and cost)
- Transfer Summary (when a patient is transferred mid-treatment from one facility to another)
“Incomplete IPD submissions are the single biggest driver of adjudication rework. A 25-point checklist is not bureaucracy; it is your fastest path to settlement.”
The Complete OPD Claims Document Checklist (15 Document Classes)
OPD claims require up to 15 document classes covering the consultation, any diagnostics ordered, and the pharmacy visit. Each class is mandatory; there is no partial approval for OPD files.
Consultation and Pharmacy Documents (OPD)
- Doctor’s Prescription (dated, signed, and stamped; must name the patient and specify diagnosis or symptoms)
- Clinic / Hospital Receipt (official receipt from the treating facility confirming consultation fee paid)
- Pharmacy Bill (itemised bill from a licensed pharmacy; medicines must correspond to the prescription)
- Specialist Referral Letter (if the OPD visit is to a specialist referred by a general practitioner)
- Teleconsultation Record (for digital-first OPD claims: platform-generated consultation summary and invoice)
Diagnostic and Lab Documents (OPD)
- Lab Report (original signed report from an accredited diagnostic centre; must include reference ranges)
- Radiology Report (X-ray, MRI, CT scan, or ultrasound report with radiologist interpretation)
- Diagnostic Centre Receipt (proof of payment for all investigations ordered)
- Doctor’s Order for Investigations (the prescription or request slip that authorised the diagnostic test)
- Dental / Optical Prescription (for vision or dental OPD claims; must specify the treating dentist or optometrist)
Identity and Policy Documents (OPD)
- Duly Completed OPD Claim Form (insurer- or TPA-specific; all fields signed and dated)
- KYC Documents of Insured (government-issued photo ID)
- Policy / Member ID Card Copy (confirms active OPD coverage)
- Insured’s Bank Account Details (for reimbursement; cancelled cheque or passbook copy)
- Pre-Authorisation Approval (if the specific OPD benefit requires prior TPA approval under the policy)
IPD vs OPD: Side-by-Side Comparison
IPD and OPD claims differ in admission threshold, document volume, processing timeline, and adjudication complexity. The table below maps the key differences so document controllers can apply the right checklist immediately.
| Parameter | IPD Claim | OPD Claim | Edge Cases / Notes |
|---|---|---|---|
| Admission Threshold | 24+ hours inpatient | No overnight stay | Day-care: under 24 hrs but classified as IPD if listed in policy |
| Document Volume | Up to 25 classes | Up to 15 classes | Complex IPD (surgery, ICU) may exceed 25 classes |
| Clinical Anchor Doc | Discharge Summary | Doctor’s Prescription | OPD without prescription is auto-rejected |
| Pre-Authorisation | Mandatory (cashless) | Policy-dependent | Some OPD benefit riders require prior approval |
| Average Processing Time (clean file) | 7 to 15 working days | 3 to 7 working days | TPAs process 98% of clean claims within 30 days |
| Fraud Risk Profile | Higher (billing inflation, unnecessary procedures) | Moderate (duplicate bills, forged prescriptions) | AI flag rates are higher for IPD due to bill complexity |
| KYC Required | Yes | Yes | Mandatory for both claim types across all TPAs |
| Settlement Mode | Cashless or Reimbursement | Reimbursement (typically) | Some network OPD centres offer cashless OPD |
The Top 5 Reasons TPAs Reject Health Insurance Claims
The most common TPA rejection reasons are incomplete documentation, mismatched patient details across documents, late intimation, policy exclusion violations, and unanswered adjuster queries. Knowing these in advance lets your team intercept failures before submission.
“OPD claims may look simpler, but a missing prescription or KYC document triggers the same rejection workflow as a missing discharge summary in an IPD file.”
1. Incomplete or Missing Documents. This is the single most controllable rejection driver. A single absent class from the checklist above halts adjudication entirely. IRDAI data for FY24 shows documentation errors sit within the broader 11% rejection rate, which amounts to Rs 15,100 crore in disallowed payouts.
2. Mismatched Patient Details Across Documents. Name spelling, date of birth, or policy number discrepancies between the claim form, hospital bill, and KYC documents trigger a query loop. Every document in the file must carry identical patient identifiers.
3. Late Claim Intimation. Most policies require intimation to the TPA within 24 hours of emergency admission and 72 hours before planned hospitalisation. Per IRDAI guidelines, failure to intimate on time gives the insurer grounds for outright rejection, even on a clinically valid claim.
4. Unanswered Adjuster Queries. According to FY24 claims data analysis, 18% of rejections occur simply because the policyholder or hospital did not respond to the TPA’s additional document request (ADR). A 24-to-48-hour response window is best practice.
5. Policy Exclusion Violations. Pre-existing condition waiting periods, OPD benefit caps, and non-covered procedures (cosmetic surgery, infertility treatment, specific consumables) account for a combined 25% of rejections in FY24 data. The document controller’s role is not to assess coverage, but to flag these risk signals early so the adjuster can review before the file is locked.
How InterPixels Auto-Classifies All 40 Document Types
InterPixels uses AI-powered document classification to automatically identify and sort all 40 IPD and OPD document classes at intake, reducing manual triage time and flagging missing documents before adjudication begins. Research from Fullerton Health’s 2025 multi-stage pipeline study demonstrated that a comparable hybrid OCR and vision-language model architecture achieved over 95% document-type classification accuracy and 87% field-level extraction across nine Asia-Pacific markets, at under 2 seconds per document.
McKinsey (2025) reports that AI-driven claims routing improves assignment accuracy by 30% and can reduce claim processing times by up to 40%. These gains come specifically from eliminating the manual document identification step that sits at the start of every claims queue.
In practice, teams building AI classification pipelines for health insurance documents find that the hardest classification problems are not the common documents (hospital bills, prescriptions) but the edge cases: GISPA declarations, implant stickers, teleconsultation records, and domiciliary treatment forms. These low-frequency documents are precisely the ones most likely to be mislabelled by manual reviewers under volume pressure.
InterPixels Document Classification Architecture
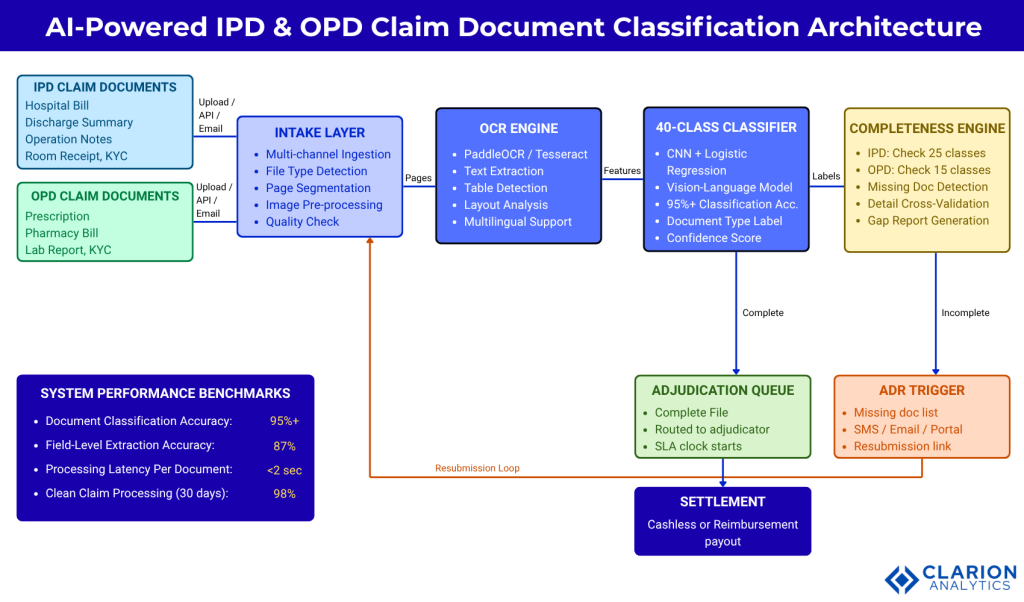
Caption: Claim documents enter via upload, API, or email. The OCR engine extracts text and structural features. The 40-class AI classifier assigns a document type label to each page. The completeness engine checks the label set against the IPD (25-class) or OPD (15-class) checklist and either routes the file to adjudication or triggers an automated Additional Document Request (ADR) to the submitting party, with specific missing documents listed.
“Auto-classification does not replace your claims team. It removes the part of their job that a machine does faster and more consistently.”
Frequently Asked Questions
What documents are required for an IPD health insurance claim in India?
An IPD health insurance claim requires up to 25 document classes, with the non-negotiable core being: the itemised hospital bill, discharge summary, completed claim form, KYC documents, and policy member card. Surgical claims add operation notes, anaesthesia records, and implant invoices. Death or accident claims add the death summary, post-mortem report, and FIR or MLC certificate.
How is OPD claims processing different from IPD at a TPA?
OPD claims do not require a discharge summary or pre-authorisation (in most policies). The anchor document is the doctor’s prescription, which must match the pharmacy bill and any diagnostic orders. OPD files carry 10 to 15 document classes versus 20 to 25 for IPD. Processing time is shorter (3 to 7 working days for a clean file), but the same completeness rules apply.
What are the most common reasons a TPA rejects a health insurance claim?
The five most common TPA rejection reasons are: (1) missing or incomplete documents, (2) patient detail mismatches across the file, (3) late claim intimation beyond the policy window, (4) unanswered adjuster queries (responsible for 18% of rejections per FY24 IRDAI data), and (5) policy exclusion violations including waiting period breaches and non-covered procedures.
Can OPD claims be submitted without a doctor’s prescription?
No. A signed and dated doctor’s prescription is the mandatory anchor document for any OPD claim. Without it, the pharmacy bill and diagnostic reports cannot be validated as medically necessary, and the claim will be rejected at intake. Teleconsultation OPD claims require a platform-generated consultation summary that serves the equivalent function.
How does AI document classification reduce health insurance claim rejections?
AI document classification eliminates two of the top five rejection drivers: missing documents (flagged at intake before submission) and mismatched details (cross-validated automatically across all pages). Research on Asia-Pacific claims pipelines shows 95%+ classification accuracy is achievable in production. McKinsey (2025) reports up to 40% reduction in processing times for AI-augmented claims teams.
Build a Rejection-Proof Claims Operation
Three insights drive everything in this guide. First, the IPD and OPD document checklists are not interchangeable: each claim type has a distinct set of required classes, and a single missing document in either category halts adjudication completely. Second, the top five rejection reasons are all preventable at the document submission stage, before the file ever reaches an adjudicator. Third, AI-powered document classification addresses the two most common rejection triggers simultaneously, at a speed and consistency no manual team can match at scale.
With Rs 30,000 crore in health insurance claims rejected or repudiated in FY2024-25 and IRDAI tightening its oversight of TPA operations, the operational cost of incomplete documentation has never been higher. Download the InterPixels IPD and OPD Claims Document Checklist to give your team a single reference that covers all 40 document classes. Or explore how InterPixels can automate classification for your existing claims queue.
Which document type causes the most rework in your current queue?