table of contents
Health insurance claims processing time is the elapsed time between a TPA or insurer receiving a complete claim submission and issuing a payment decision. In the Asia Pacific region, this ranges from under 5 minutes for AI-automated pipelines to 3-5 days for manual inpatient workflows. The APAC industry average sits at approximately 25 minutes per claim for outpatient processing in 2026.
Why APAC TAT Is a Competitive Battleground Right Now
Asia Pacific’s health insurance TPA market is growing at more than 9.62% CAGR through 2030, driven by rising middle-class populations, expanding digital health infrastructure, and increasingly assertive regulators. Processing speed is no longer a back-office metric.
India’s Insurance Regulatory and Development Authority (IRDAI) now mandates cashless claim authorization within one hour and final discharge approval within three hours, enforceable from July 2024. Miss that window and the insurer pays interest at the prevailing bank rate plus two percent for every day of delay. Speed has acquired a price tag.
Meanwhile, Experian Health’s 2024 State of Claims found that 65% of healthcare leaders consider claims management more complex than before the pandemic, and 48% still review denials manually. That figure represents an enormous operational liability for any TPA still relying on manual workflows.
“Processing speed is no longer a back-office metric. In APAC, it is a regulatory obligation with a financial penalty attached to every hour of delay.”
APAC Country Benchmarks: India, Malaysia, Indonesia, and Singapore
The four most benchmarked APAC markets show distinct TAT profiles shaped by regulatory environment, digital maturity, and TPA consolidation. The table below maps current state against AI-enabled targets.
| Country | Manual Avg TAT | AI-Enabled TAT | Regulatory Benchmark | Key Driver |
|---|---|---|---|---|
| India | 35-45 min (OPD) | 5-8 min | IRDAI: 1 hr cashless auth / 3 hr discharge (2024) | Regulatory pressure + NHCX digital exchange |
| Malaysia | 25-35 min (OPD) | 6-10 min | Bank Negara: 24 hr reimbursement target | Private hospital network digitization |
| Indonesia | 30-40 min (OPD) | 8-12 min | OJK: ongoing digital health framework | BPJS scale + AI adoption via Pacific Cross / Qantev |
| Singapore | 15-20 min (OPD) | 3-5 min | MAS / MOH: real-time pre-auth expected | Mature TPA market, highest digital penetration |
Sources: IRDAI Master Circular 2024; Next Move Strategy Consulting APAC TPA Market Reports 2025; The Digital Insurer; TrueCover production data.
India
India’s IRDAI PPHI Regulations 2024 represent the most prescriptive TAT framework in the region. The one-hour cashless authorization rule forced every major TPA to invest in digital pre-authorization infrastructure before July 2024. The compliance result was visible: complaints about cashless delays fell from 1.87% of total grievances in FY 2024-25 to just 0.39% in H1 of FY 2025-26, according to Finance Minister Nirmala Sitharaman’s parliamentary statement.
The India TPA market is valued at USD 5.91 billion and growing to USD 9.29 billion by 2030, with consolidation such as Medi Assist acquiring Paramount Health Services in August 2024 driving scale efficiencies that directly compress TAT.
Malaysia
Malaysia’s TPA ecosystem sits in a mid-tier performance band. Private hospital network digitization has shortened OPD TAT for major group insurance clients, but rural and panel hospitals still generate document bottlenecks that add 15-20 minutes to manual workflows.
Indonesia
Indonesia is the fastest-moving market by adoption velocity. The Indonesia TPA market is expected to grow from USD 1.66 billion in 2024 to USD 5.32 billion by 2030 at a 20.6% CAGR. In March 2024, Pacific Cross partnered with Qantev to deploy AI-powered claims and fraud detection across five APAC countries including Indonesia, a signal that the market is leapfrogging legacy infrastructure.
Singapore
Singapore operates the region’s most mature digital claims environment. The Singapore TPA market was valued at USD 3.22 billion in 2023 and is forecast to reach USD 7.53 billion by 2030. The key advantage is not just technology but the ecosystem: a concentrated hospital network with standardized digital records cuts document-ingestion time before AI even starts its work.
“Singapore’s advantage is not just faster AI. It is a standardized hospital record ecosystem that eliminates the document-chaos that inflates TAT everywhere else in APAC.”
Claim-Type TAT Benchmarks: IPD vs OPD
Claim type is the single biggest predictor of TAT variance across APAC. Inpatient and outpatient claims have fundamentally different document complexity profiles.
| Claim Type | Manual APAC Avg | AI-Automated | Key Bottleneck | AI Intervention |
|---|---|---|---|---|
| OPD (Outpatient) | 1-2 days / 25 min per claim | 5-10 minutes | Document verification, eligibility check | OCR + NLP + rules engine automates 80% |
| IPD (Inpatient) | 3-5 days | 4-8 hours | Clinical record complexity, multi-specialty discharge summary | NLP clinical entity extraction + human-in-loop for complex cases |
| Pre-authorization | 2-4 hours | Under 1 hour (IRDAI mandate) | Manual policy-rules lookup | Real-time rules engine against policy terms |
Note: ‘AI-Automated’ figures reflect TPAs with full ML + RPA pipeline deployment. Partial automation achieves intermediate results.
IPD claims will always require human review at the adjudication stage for complex or high-value cases. The AI opportunity here is not full automation but compression: reducing the human reviewer’s preparation time from hours to minutes by pre-populating structured summaries from clinical documents.
How AI Compresses Every Stage of the Claims Pipeline
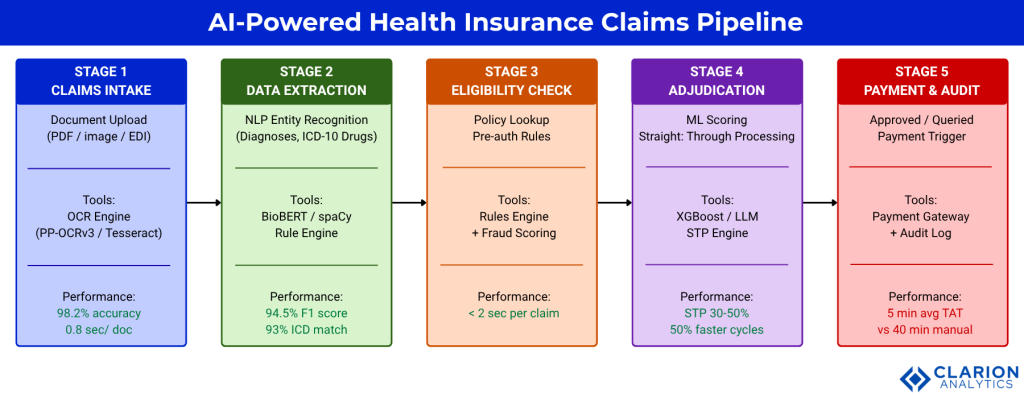
The shift from 40-minute manual processing to under 5 minutes does not come from a single technology. It comes from automating four sequential stages. Research published in the International Journal of Science and Research Archives (2025) found that AI-driven Intelligent Document Processing combining ML, NLP, and RPA reduces document processing time by 80% and error rates by 90%. Here is how each stage contributes.
Stage 1: Document Ingestion via OCR
OCR converts scanned invoices, discharge summaries, and handwritten prescriptions into machine-readable text. Modern implementations like PP-OCRv3 achieve 98.2% accuracy at 0.8 seconds per document according to a 2025 ACM DEBAI study. That replaces 8-12 minutes of manual data entry per claim.
Stage 2: Data Extraction via NLP
NLP models read the structured text and extract clinical entities: diagnosis codes, drug names, procedure codes, and attending physician details. BioBERT-based models achieve 94.5% F1 on medical entity recognition and 93% accuracy on ICD-10 code matching. This stage replaces manual coding, the most error-prone step in manual processing.
Stage 3: Eligibility and Rules Engine
The extracted entities are cross-referenced against the policy in real time. A rules engine checks coverage limits, pre-existing condition exclusions, and network hospital status in under 2 seconds. This is where the IRDAI one-hour pre-authorization mandate is met: the rules engine fires instantly rather than waiting for a human to open the policy document.
Stage 4: Adjudication and Payment
Straight-through processing (STP) is the final frontier. Deloitte’s 2025 AI Outlook benchmarks STP at 30-50% on standard personal lines. Claims that pass all automated checks are approved and routed to payment without human intervention. Claims that flag anomalies go to a human reviewer with a pre-populated decision brief, cutting review time from 30 minutes to under 5.
TPA Performance Comparison: Manual vs Industry Average vs AI-Automated
The gap between manual and AI-automated processing is not marginal. It is an 87.5% reduction in per-claim handling time and the basis for a board-ready ROI case.
| Approach | Avg Per-Claim Time | Key Strength | Best Used When | Operational Cost |
|---|---|---|---|---|
| Manual Processing | 40 minutes | Full human judgment; handles edge cases and fraud nuances naturally | Complex IPD claims requiring clinical expertise and disputed cases | Baseline (100%) |
| APAC Industry Average (Partial Automation) | 25 minutes | Handles high volumes with rule-based automation; reduces data entry | Mid-size TPAs with legacy systems investing incrementally in automation | 60-75% of manual |
| AI-Automated (Full Pipeline) | 5 minutes | Full-stack ML + NLP + RPA with STP; fraud detection embedded; scales infinitely | High-volume OPD claims; group health TPAs processing 10,000+ claims/day | 65-80% of manual |
| TrueCover Production (APAC) | 5 minutes | Live APAC production data; matches full AI-automated benchmark with local document formats | Reference data point for APAC-specific deployment validation | Verified production |
Source: TrueCover production data; McKinsey AI Insurance Report 2025; Deloitte AI Outlook 2025; APAC industry averages compiled from Next Move Strategy Consulting and Bonafide Research 2025.
“An 87.5% reduction in per-claim handling time is not an incremental improvement. It is the difference between a cost centre and a competitive weapon.”
TrueCover Production Data: From 40 to 5 Minutes
Benchmark data from research firms describes what AI can achieve. Production data from a running APAC TPA describes what it actually delivers. TrueCover’s deployment reduced average per-claim processing time from 40 minutes to 5 minutes across its APAC book of business.
The pipeline covers document ingestion, NLP-based data extraction, rules-engine eligibility checks, and ML-driven adjudication. The 5-minute figure includes the time for asynchronous OCR processing of multi-page hospital bills, which is the most document-heavy step in APAC workflows due to the prevalence of non-standardized billing formats across the region’s hospital networks.
The second data point worth noting is TAT versus the industry average. Where the APAC industry average for OPD claims sits at approximately 25 minutes, TrueCover’s AI pipeline delivers the same adjudication decision at 5 minutes. For a TPA processing 50,000 claims per month, that difference equals roughly 16,667 staff-hours recovered every month and reallocated to exception handling and quality assurance. Validated against McKinsey’s 2025 AI Insurance analysis, which found AI systems cutting complex liability assessment time by 23 days for Aviva’s UK claims operation, the APAC production data is consistent with global AI performance patterns.
Implementation Realities: What Teams Building This Actually Find
In practice, the biggest barrier to AI claims automation in APAC is not the model quality. It is the data. Hospital billing formats vary not just by country but by hospital network, sometimes by individual facility. A discharge summary from a Jakarta private hospital and one from a Jakarta public hospital may share almost no formatting conventions.
Teams building this pipeline typically find they spend 60-70% of the initial project timeline on document pre-processing standardization rather than on model training. A 2025 IDP research paper confirmed that organizations taking a phased approach to deployment starting with claims processing before expanding to underwriting and fraud detection achieved 40% cost savings while avoiding the system bottlenecks that hit teams that attempted a big-bang deployment.
The multilingual dimension adds complexity specific to APAC. Medical records in Malaysia arrive in Bahasa Malaysia and English; Indonesian records mix Bahasa Indonesia with Dutch-derived medical terminology; Thai records may include transliterated drug names. A 2025 ACM study on intelligent claim models demonstrated that BioBERT-based NLP with ICD-10 knowledge graphs handles multilingual entity extraction at 94.5% F1, making it the current standard for APAC deployments.
The fraud dimension is non-trivial. AI-powered fraud detection must be trained on local patterns. Overcharging by public hospitals is the dominant fraud vector in China and Indonesia; upcoding of procedures is more common in private networks in Malaysia and Singapore. A single fraud model trained on US insurance data will underperform on APAC claims without fine-tuning.
“The AI model is ready. The real work in APAC claims automation is the 60-70% of project time spent standardizing document formats before the model can begin learning.”
Frequently Asked Questions
What is the average health insurance claims processing time in Asia Pacific?
The APAC industry average for outpatient (OPD) health insurance claims is approximately 25 minutes per claim in 2026 using partial automation. Manual-only TPAs average 35-45 minutes depending on document complexity. AI-automated pipelines compress this to under 5 minutes. Inpatient (IPD) claims take 3-5 days manually and 4-8 hours with AI due to clinical document complexity.
How does AI reduce insurance claim turnaround time?
AI reduces TAT by automating the four most time-intensive stages: OCR ingests documents at 0.8 seconds each with 98.2% accuracy; NLP extracts clinical entities at 94.5% F1; a rules engine runs eligibility checks in under 2 seconds; and an ML adjudication model processes standard claims via straight-through processing (STP) at rates of 30-50%, removing the need for human review on the majority of claims. The net result is an 87.5% reduction in per-claim handling time per Deloitte’s 2025 benchmark.
What does IRDAI require for cashless claim processing time in India?
Under the IRDAI Master Circular on Health Insurance Business (2024), insurers must grant initial cashless authorization within one hour of receiving all required documents from the hospital. Final discharge authorization must be granted within three hours of the discharge request. Delays attract interest at the prevailing bank rate plus two percent per day. These timelines became mandatory from July 31, 2024.
What is the difference between IPD and OPD claims processing time?
Outpatient (OPD) claims involve single-visit documents, typically a prescription and a bill, and are processed in 1-2 days manually or 5-10 minutes with AI. Inpatient (IPD) claims include discharge summaries, operative notes, nursing records, and multi-specialist consultation reports that span multi-day admissions. IPD claims average 3-5 days manually and 4-8 hours with AI assistance due to the volume and complexity of clinical documentation requiring review.
How do APAC TPAs compare on claims processing speed?
Singapore achieves the fastest TAT at 15-20 minutes manually and 3-5 minutes with AI, benefiting from standardized hospital records and a mature digital ecosystem. India is the most regulated market with IRDAI mandating sub-one-hour cashless authorization. Indonesia is the fastest-growing in AI adoption velocity at 20.6% CAGR for the TPA market. Malaysia sits in a mid-tier performance band, closing the gap through private hospital network digitization. All markets show 80%+ TAT compression when full AI pipelines are deployed.
The Three Insights That Change How You Operate
“The APAC TPA that closes the gap between its current TAT and the 5-minute benchmark will not just satisfy regulators. It will define the competitive standard for the next decade.”
First, regulatory pressure is the catalyst, not the destination. IRDAI’s 2024 mandates are the floor, not the ceiling. The TPAs building AI pipelines today are not just complying; they are creating operational moats that take 18-24 months for competitors to replicate. Second, the AI stack is not experimental. The benchmarks are proven: 98.2% OCR accuracy, 94.5% NLP F1, 30-50% STP rates. These are production figures validated by McKinsey (2025) and confirmed by TrueCover’s own APAC deployment data. Third, the constraint is no longer technology. It is data standardization. The TPA that invests in structured document pipelines across its hospital network today will be the one whose AI models outperform in 2027.
If you are a COO benchmarking TAT, the question is no longer whether AI works. The question is how many months of claim-processing cost you are willing to pay while your competitors close the 35-minute gap.