table of contents
A third-party administrator (TPA) in health insurance is a licensed company that manages claims processing, pre-authorisation, and member services on behalf of an insurer. The TPA sits between the policyholder and the healthcare provider, running the operational layer so the insurer can focus on underwriting and risk. Across Asia Pacific, TPAs handle an estimated 60 to 70% of corporate group health claims by volume, making them the invisible backbone of employer-sponsored health coverage.
Why Asia Pacific’s Health Insurance Boom Created a TPA Industry
The global TPA market reached USD 432 billion in 2024 and is forecast to hit USD 886 billion by 2033, growing at an 8.3% CAGR, according to Straits Research (2025). Asia Pacific is the fastest-growing region in that outlook. The reason is structural: as millions of workers across India, Malaysia, and Indonesia gained access to employer health plans, insurers found they could not scale their operations fast enough to handle the resulting claims volume. TPAs exist to solve exactly that problem.
TPA health insurance Asia Pacific is not a niche category. In India alone, the TPA sector processes tens of billions of rupees in claims annually, with Medi Assist commanding a 36.6% share of the group segment after its 2024 acquisition of Paramount TPA. Understanding how these administrators operate, how they are licensed, and how AI is reshaping their workflows is now essential knowledge for any operations leader running a health insurance back-office in the region.
The TPA’s Role in the Health Insurance Ecosystem
A TPA is not an insurer and does not carry underwriting risk. It processes claims, manages hospital networks, handles pre-authorisation, and reports claims data to the insurer under a formal service agreement.
The TPA model emerged in the United States in the 1970s under managed care legislation. India adopted it formally in 2001 when IRDAI issued its first TPA regulations, followed by Malaysia and Indonesia building their own frameworks. Today, TPAs perform four core functions across the region.
First, they manage hospital networks. A TPA signs empanelment agreements with hundreds or thousands of hospitals, negotiating rates and cashless payment protocols. Second, they handle member services, including ID card issuance, helpline support, and eligibility queries. Third, they run the claims lifecycle from intake through settlement. Fourth, they generate data and analytics reports that help insurers track loss ratios, fraud trends, and provider behaviour.
“A TPA earns its fee not by controlling risk but by controlling the cost of administering risk. Speed and accuracy are its only competitive moat.”
How a Health Insurance Claim Actually Flows Through a TPA
A TPA claim moves through five stages: intake and FNOL, document validation, adjudication against policy rules, fraud screening, and payment settlement. Cashless claims complete stages 1 through 5 in hours. Reimbursement claims typically settle within 30 days under IRDAI guidelines.
Stage 1: Claim Intake and FNOL
The policyholder or hospital initiates a First Notice of Loss through a portal, mobile app, or helpline. The system captures member ID, policy number, diagnosis codes, and the name of the treating provider. Modern TPA platforms validate eligibility in real time against the insurer’s policy database.
This handler validates the three mandatory FNOL fields, then publishes a structured event to an event bus. Downstream services for document validation, adjudication, and fraud scoring each subscribe independently. The pattern decouples stages so a slow fraud check does not block payment of a clean, low-risk claim.
Stage 2: Document Validation
The TPA receives scanned hospital bills, discharge summaries, and clinical notes. OCR extracts text. NLP identifies ICD-10 diagnosis codes, procedure codes, and charged amounts. The system flags missing fields or mismatched data before the claim reaches adjudication.
This pipeline sends a scanned hospital bill to Azure’s pre-trained invoice model. It returns structured fields such as patient name, total charged, and service date directly as JSON. The TPA adjudication engine receives clean, typed data rather than unstructured text, cutting manual keying errors and speeding cycle time. A 2024 study in the Journal of Artificial Intelligence Research found that phased AI document processing deployments produced 40% cost savings in insurance claims operations.
“Teams building AI document intake typically find the first 80% of extraction accuracy is fast. The last 20%, covering handwritten notes and non-standard bill formats, is where most of the implementation effort lives.”
Stage 3: Adjudication
The adjudication engine applies the insurer’s policy rules: deductibles, co-payments, sub-limits, waiting periods, and exclusions. Smart policy engines embed payer-specific rules and update in real time as product terms change. The engine approves, denies, or flags for manual review.
Stage 4: Fraud Screening
Fraud screening runs in parallel with adjudication. ML anomaly models score each claim against behavioural baselines. A 2024 IBM Research paper published in Nature Scientific Reports demonstrated that collaborative AI systems using knowledge graphs can detect non-compliant claims without requiring labelled fraud training data. For APAC TPAs, where labelled fraud datasets are scarce, this approach is practically significant.
Stage 5: Settlement and Payment
Approved cashless claims route directly to the hospital’s account. Approved reimbursement claims credit the policyholder. Both paths trigger a confirmation notification to the member. IRDAI requires cashless pre-authorisation within one hour of the request and final discharge authorisation within three hours under its 2024 Master Circular on Health Insurance Business.
TPA vs Insurer vs Broker: Who Does What?
The three entities in a health insurance value chain play distinct roles. Confusing them is one of the most common errors made by corporate HR teams setting up group health schemes.
| Entity | Key Strength | Best Used When |
|---|---|---|
| TPA | Claims operations, hospital network management, adjudication speed, member services | Insurer needs to outsource the full claims back-office and reduce operational headcount |
| Insurer | Underwriting, risk pricing, product design, regulatory capital holding | Carrier wants end-to-end control and direct claims settlement without outsourcing |
| Broker | Multi-insurer comparison, policy placement, client advice, renewal management | Employer needs independent guidance on plan design and does not want to deal with insurers directly |
| In-house TPA (Insurer-owned) | Integrated data, lower per-claim cost at scale, tighter quality control | Large insurer with sufficient volume to justify building and maintaining its own claims platform |
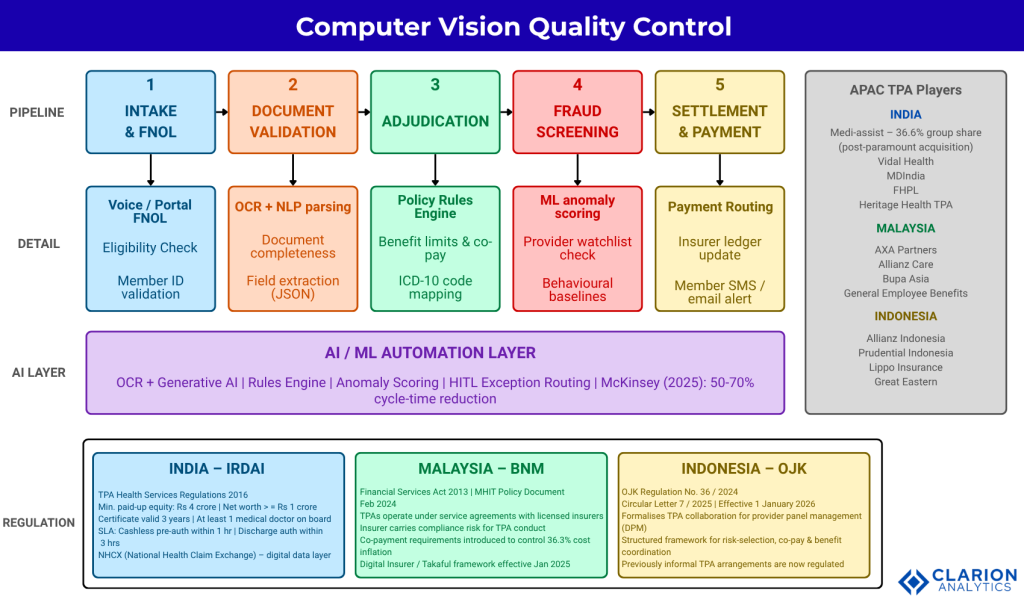
TPA Licensing by Country: India, Malaysia, and Indonesia
In India, TPAs are licensed by IRDAI under the 2016 TPA Health Services Regulations, requiring Rs 4 crore paid-up capital. In Malaysia, BNM regulates health insurance and takaful operators under the Financial Services Act 2013, with TPA activities covered under service agreements with licensed insurers. In Indonesia, OJK governs TPA collaboration under OJK Regulation No. 36 of 2024, with Circular Letter 7/2025 effective January 2026.
| Country | Regulator | Key Instrument | Capital / Key Requirement |
|---|---|---|---|
| India | IRDAI | TPA Health Services Regulations, 2016 | Rs 4 crore paid-up equity; net worth >= Rs 1 crore; Certificate renewable every 3 years; at least one medical doctor on the board |
| Malaysia | BNM | Financial Services Act 2013; MHIT Policy Document (Feb 2024) | TPAs operate under service agreements with licensed insurers; BNM oversight focuses on insurer accountability for TPA conduct; Digital Insurer/Takaful framework from Jan 2025 |
| Indonesia | OJK | OJK Reg No. 36/2024; Circular 7/2025 (eff. Jan 2026) | Insurance entities may collaborate with third-party administrators for provider management (DPM); TPA must comply with new health insurance product standards |
India: IRDAI Licensing Requirements
IRDAI’s TPA Health Services Regulations (2016) are the most detailed TPA licensing framework in the region. Only companies incorporated under the Companies Act 2013, with health services as their sole stated objective, may apply. The application fee is Rs 1 lakh, and IRDAI grants a three-year Certificate of Registration after approving the application. TPAs must commence operations within 12 months of registration. The 2024 Master Circular further mandated that insurers achieve 100% cashless settlement, with pre-authorisation decisions within one hour.
India’s NHCX (National Health Claim Exchange) is the digital layer through which TPAs, insurers, and hospitals exchange structured claim data. Compliance with NHCX standards is becoming a de facto operational requirement for TPAs working with major general insurers.
Malaysia: BNM Framework
Bank Negara Malaysia regulates health insurance and takaful (MHIT) under its February 2024 Policy Document on MHIT Business. TPAs in Malaysia operate as service providers to licensed insurers and takaful operators rather than as independently licensed entities. BNM holds the insurer accountable for TPA conduct, which means the insurer carries the compliance risk. BNM’s 2024 framework also introduced co-payment requirements for medical reimbursement policies, aiming to contain medical cost inflation that rose 36.3% cumulatively from 2020 to 2022.
Indonesia: OJK Regulation
OJK Regulation No. 36/2024 and its implementing Circular Letter 7/2025 (effective January 2026) allow insurance entities to establish or collaborate with third-party administrators for provider panel management (DPM). This is a significant formalisation: previously, TPA arrangements in Indonesia operated under informal service agreements. The new framework requires that TPA collaboration meet OJK’s standards for risk-selection, co-payment, and coordination of benefits.
“Regulatory divergence across IRDAI, BNM, and OJK is the single biggest compliance headache for any TPA operating across multiple APAC markets. A single playbook cannot cover all three.”
Major TPA Players in Asia Pacific
India’s TPA market is dominated by Medi Assist (36.6% group segment share following its 2024 acquisition of Paramount TPA), Vidal Health, MDIndia, and FHPL. In Southeast Asia, the landscape is dominated by global insurer-owned TPA arms rather than independent specialists.
The landmark deal in 2024 was Medi Assist’s acquisition of Paramount TPA for INR 311.8 crore, making it one of the largest TPA transactions in Indian history. The combined entity manages premiums for 30 insurers and over 3,000 group customers. Medi Assist has explicitly flagged AI and ML as the technology layer that will drive post-merger efficiency gains.
In Malaysia, health TPA services are embedded within the operations of Allianz, AXA Partners, Bupa Asia, and Generali Employee Benefits. These global players bring technology investment and cross-border network capabilities that independent TPAs in the region cannot easily match. Indonesia follows a similar pattern, with Lippo Insurance, Prudential, and Allianz dominating corporate health administration.
How AI Is Transforming TPA Operations in 2026
AI is reshaping TPA operations at three points: intake automation via OCR and NLP, adjudication acceleration through rules engines and ML models, and fraud detection using anomaly scoring. According to McKinsey (2025), AI-driven claims automation can reduce processing time by 50 to 70%. The firm also notes that agentic AI accounted for 21% of public AI deployments in insurance in Q4 2025, with the majority focused on claims management.
Intake Automation
Voice-based FNOL through IVR and chatbot is now standard at tier-1 Indian TPAs. NLP parses the member’s description and auto-populates the claim form. OCR handles scanned hospital bills, prescription images, and discharge summaries. The practical gain is that intake processing time drops from hours to minutes for straight-through cases.
Adjudication and Policy Rules Engines
Smart policy engines embed coverage rules, benefit limits, and ICD-10 code mappings directly into the adjudication engine. According to a 2025 ResearchGate paper on AI in healthcare claims adjudication, LLMs now auto-generate denial justification letters and triage complex cases to human reviewers, reducing administrative burden significantly. The engine learns from past decisions, continuously improving its routing accuracy.
Fraud Detection and Anomaly Scoring
Traditional rule-based fraud detection flags known patterns. ML-based anomaly scoring detects statistical deviations from provider and member baselines that rule-sets miss entirely. A 2024 IBM Research study published in Nature Scientific Reports demonstrated that a collaborative AI system using knowledge graphs detects non-compliant claims without requiring labelled fraud training data. For APAC TPAs, where labelled fraud datasets are scarce, this approach is practically significant.
The Pricing Model Problem
McKinsey’s 2026 analysis identifies a critical tension: most TPA contracts are still priced on headcount or per-transaction volume. When AI automates claims processing, the TPA’s cost falls but so does its revenue under these models. As McKinsey notes, per Investment Executive (2026), “the next phase of the subsector will be defined less by whether TPAs adopt AI and more by how they evolve their pricing models.” Operations leaders need to anticipate this tension now, not after automation has already eroded their margin.
“Adopting AI in claims processing is the easy part. Repricing your TPA contracts to reflect outcome-based value rather than activity volume is where the real commercial work begins.”
Frequently Asked Questions About TPAs in Health Insurance
What does a TPA do in health insurance?
A TPA manages claims processing, hospital network empanelment, pre-authorisation, and member services on behalf of a health insurer. It acts as the operational back-office between the policyholder, the hospital, and the insurer. The TPA does not carry insurance risk; it earns a service fee for processing speed and accuracy.
How is a TPA different from a health insurer?
An insurer underwrites risk, holds regulatory capital, and is ultimately liable for claim payments. A TPA administers the process of receiving, validating, adjudicating, and paying claims. Many insurers outsource this operational layer entirely to a TPA. Others build in-house TPA capabilities. Some large TPAs, particularly in India, manage claims for 20 or more different insurance companies simultaneously.
How long does it take a TPA to process a health insurance claim?
Under IRDAI’s 2024 Master Circular, cashless pre-authorisation must be granted within one hour of request. Final discharge authorisation must follow within three hours. Reimbursement claims for non-cashless treatment must be settled within 30 days. AI-powered TPAs routinely beat these timelines for straightforward claims with clean documentation.
Do I need IRDAI registration to operate as a TPA in India?
Yes. Any entity providing health TPA services in India must hold a Certificate of Registration from IRDAI under the 2016 TPA Health Services Regulations. The applicant must be incorporated under the Companies Act 2013, have health services as its sole stated business objective, hold a minimum Rs 4 crore paid-up equity, and maintain net worth of at least Rs 1 crore at all times. The certificate is valid for three years and must be renewed.
How is AI changing how TPAs process claims?
AI transforms TPA operations at three stages. At intake, OCR and NLP replace manual data entry for claim forms and hospital bills. At adjudication, ML rules engines auto-approve or deny claims against policy terms without human review for straight-through cases. At fraud screening, anomaly models detect unusual billing patterns that rule-based systems miss. McKinsey estimates these combined changes reduce claims cycle time by 50 to 70%.
Three Things Every TPA Operations Leader Should Take Away
First, the regulatory landscape in India, Malaysia, and Indonesia is converging toward cashless-first, digitally-enforced SLAs. IRDAI’s one-hour pre-auth rule, BNM’s co-payment framework, and OJK’s 2026 health insurance standards all push in the same direction: faster, more transparent, technology-driven claims handling. TPA ops teams that are still running manual document queues are already behind.
Second, AI adoption in claims is no longer optional. McKinsey estimates early AI leaders in insurance generate six times the total shareholder returns of their AI-laggard peers. For TPAs, this gap is even more pronounced because their entire business model is built on operational efficiency. The question is not whether to automate but how to sequence it and how to restructure contracts to capture the value.
Third, APAC consolidation is accelerating. Medi Assist’s acquisition of Paramount TPA in 2024 signals what the Indian market will look like in five years: a small number of large, technology-driven TPAs serving dozens of insurers, and a long tail of specialists serving niche segments. For mid-size TPA operators, the strategic decision is whether to build, partner, or sell before that consolidation reaches them.
Automate Your TPA Document Workflow with InterPixels AI
Much of the document bottleneck described in Stage 2 of this guide, the manual keying of hospital bills, discharge summaries, and prescription data before adjudication can begin, is precisely where APAC TPAs continue to lose the most time. InterPixels AI addresses this directly. Built by Clarion Analytics in Singapore, it is a claims intelligence API trained on the 40+ document types that health insurance TPAs across India, Malaysia, and Indonesia process daily. It validates, extracts, and fraud-screens each submission at intake, returning structured JSON ready for your adjudication engine with no changes required to your existing TPA platform. If your team is still reviewing entire documents manually, the platform is worth a closer look. Contact the InterPixels team to see a live walkthrough.